|
|
 | |
PC or pancreatic
cancer
|
 |
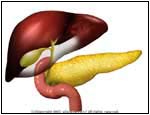
Normal |
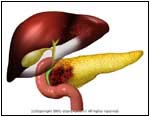
Abnormal |
| |
- The pancreas is an elongated organ
that lies transversely behind the stomach (it has a head and
tail). A section of the pancreas called the exocrine
pancreas secrets chemicals called enzymes into the duodenum
of the stomach.
- Pancreatic juices leave the pancreas via a collection of tubes called pancreatic ducts, joining juices from the gallbladder (help to digest fat) and liver, and travel to the duodenum via the common bile duct. Enzymes in pancreatic juice help break down Proteins in our food.
- Most occurrences of Pancreatic Cancer
originate in the ductal system, and are called
adenocarcinomas.
- Other parts of the pancreas produce hormones (endocrine pancreas) such as Insulin and Glucagon, which
regulate blood glucose (sugar) levels and somatostatin,
which regulates the release of other hormones (e.g., growth
hormone). These hormones do not go to the stomach, but are
directly released into the blood stream.
- Cancers affecting the endocrine
cells are called islet cell cancers.
- Pancreatic Cancers
are the 4th cause of cancer death in the United States.
- By the time Pancreatic Cancer is
diagnosed, it is often too late -- most patients die within
3-6 months.
|
 |
- Weight loss is the most common
(90%) symptom
- Fatigue and weakness
- Loss of appetite
- Nausea and vomiting
- Diarrhea or
clay-colored stool
- Abdominal pain (75%)
- Abdominal tenderness when touched
- Indigestion --
feeling bloated and heartburn
- Back pain
- Yellowish discoloration of skin and
whites of the eye (jaundice)
- Itchiness of the skin
- May feel a mass or a lump over the
pancreas
- May feel an enlarged gallbladder or
liver
- There may be fluid build up in the
abdomen (ascites)
- Depression
- Anemia -- low blood levels are
present in 60% of
patients
|
 | |
|
 |
- The general physician will consult with a
gasteroenterologist or digestive tract specialist (GI),
cancer specialist, or oncologist, radiologist, and surgeons.
- A full medical history of symptoms, risk factors,
medical surgeries, illnesses, habits, and family
history
- Medical exam may reveal jaundice, weight loss, ascites,
a mass, or enlarged liver.
- The doctor will do a stool test for the presence of
blood by using his index finger and inserting it in the
rectum to collect small stool sample.
- Blood test -- routine liver and kidney functions and a
complete blood cell count (red and white cells)
- Blood chemical such as Bilirubin, Alkaline phosphatase, Amylase, CEA, CA 19-9, pancreatic -- oncofetal antigen, and alpha-fetal Proteins are tests
that when elevated may help in diagnosing PC.
- X-Rays of abdomen
- Upper GI -- special X-Ray (Barium) will show a
outline of the esophagus and the stomach
- Ultrasound uses sound
to show the structure of the pancreas
- CAT scan (computers) and MRI (magnetic energy) show a
more detailed picture of the pancreas.
- ERCP -- done by GI. A flexible plastic camera (endoscope) is passed down the throat into the stomach and the doctor injects a dye for X-Rays. ERCP is useful in
seeing the common bile and pancreatic ducts.
- PTC -- is done by inserting a needle through the skin into the liver to inject dye, and X-Rays of the bile ducts are
taken to see blockages.
- Angiography --
done if the blood vessels supplying the pancreas need to be visualized. A dye is injected into the blood and X-Rays taken.
- Biopsy -- a piece of the cancer is taken for proper
identification
- Biopsies can be done at the same time as the ERCP by
attaching a brush to the end of the endoscope and scraping
some of the cancerous tumor cells off for review.
- Biopsy can also be done using a needle inserted into the pancreas while a CAT scan or Ultrasound guides
the radiologist.
- Biopsy is also done by surgeons using a laparoscope.
- Laparotomy refers to opening the abdomen under
anesthesia and examining its contents and the tumor.
- Biopsies are sent to a pathologist who uses a
microscope to look for cancer
cells.
|
 |
-
Not proven
but suspected:
- Sex -- males>females
- Age -- rare under 40, but risks increases with age;
average age of diagnosis is 70.
- Race -- blacks and Hawaiians > whites. Low
occurrence in Asians and Hispanics.
- Diet -- low in vegetables and fruits, high in animal
fats and meat products
- Smoking
- Diabetes
- Occupation -- petroleum and other chemicals
- Likely that there is no association between
pancreatitis (swollen, irritated pancreas), coffee, or
alcohol.
|
 |
- If the cancer is small and has not
metastasized (spread) out of the pancreas, the prognosis of
treatment (outcome) is favorable.
- The patient is admitted to a
hospital for tests and treatments
- Type of treatment depends on the
extent of metastasis and general health of the patient
- Antacids
- Insulin, if glucose
levels are high
- Glucose solutions, if blood sugars
are low.
- Painkillers such as Tylenol, Codeine, Demerol, and Morphine
- Cholestyramine or other medications
for severe itching
- Pancreatic enzymes such as Pancrease
- Medications to treat Depression may be
needed.
- Diet is usually as tolerated.
- If losing weight, consider
supplementing with high protein shakes and use of NasalGT or
GT feeding (done by putting a tube into the stomach through
the nose, or directly through the stomach).
- TPN is giving nutrients via plastic
tubing directly into the blood stream.
- Surgery -- removal of a part or all
of the pancreas and some of the surrounding structures is
often the only choice.
- Radiation -- radioactive rays can
be lethal to cancer cells. Radiation may be given before
surgery to shrink the cancer, or afterward to decrease the
chance of the cancer cells returning. Radiation can also be
useful in cases where surgery is not an option, to alleviate
symptoms such as pain.
- Chemotherapy -- uses cancer-killing
chemicals, often given in combination with other treatments
- Immunotherapy -- fights cancer by
strengthening body's own defenses.
- Clinical trials -- new treatments
tested and researched on cancer patients
- Most treatments have severe
side-effects that must be considered.
- Support for the family and patient
- If treatments are not effective,
hospice and other organizations can provide palliative or
comfort care.
|
 |
-
Contact
your physician and ask about all the options for treatment.
Call the Cancer Information Services at 1-800-4 CANCER to
find out more about clinical trials. Keep on
fighting!
|
| | |
If you want your friend to read or know about this article, Click here
 |
|
|

