|
|
 | |
Pericardial
effusion
|
 |
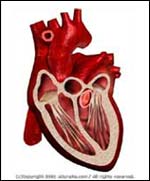
Normal |
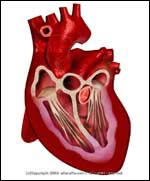
Abnormal |
| |
- The heart sits in an envelope of tissue called the pericardial sac. Under normal conditions, minimal fluid (just enough for "lubrication") is present. If, however, the pericardial sac is allowed to fill with fluid, a condition known as Pericardial Effusion
occurs.
- This can reach dangerous levels in which the heart is no longer able to pump, resulting in Cardiac Tamponade -- a life-threatening condition
that may lead to cardiac
arrest.
|
 |
- Chest pain that is usually worse with
a deep breath; pain improves by leaning forward.
- Shortness of breath
- Cough may be present
- Fainting, lightheadedness, unconsciousness, or cardiac arrest may be present in the case of Cardiac Tamponade
|
 |
- Dressler's syndrome (pericarditis
that occurs after a heart attack or after heart bypass
surgery)
- Renal failure
- Uremic pericarditis
- Trauma/Injury
- Neoplastic (cancer) pericarditis
- Infectious pericarditis
- Rheumatic fever
- Viral pericarditis
- Tuberculous pericarditis
- Radiation induced pericarditis
- Systemic lupus erythematous
- Hypothyroidism
- Rheumatoid arthritis
- In all these cases, there is pericarditis (i.e. inflamation of the pericardial tissue). This inflammation results in fluid release and build up in the pericardial sac. Pericarditis only rarely leads to actual Cardiac Tamponade.
|
 |
- Tachycardia (heart rate is
elevated usually above 100)
- Heart exam may reveal a
pericardial rub
- Tachypnea (rapid breathing)
- Pulsus paradoxus (systolic blood
pressure drops by more than 10 mm Hg during inspiration)
- Ascites (swelling of
the abdomen) and edema (leg swelling) may be
present
- Central venous pressure (may be
checked with a special catheter) is usually elevated
- Laboratory tests, e.g.,
sedimentation rate, ANA, rheumatoid factor.
- Chemistry panel to check kidney function and assess for uremic pericarditis (as well as other abnormalities). Complete blood count
and thyroid function tests should be evaluated.
- Consider TB skin testing
- Chest X-Ray shows an enlarged
cardiac silhouette
- EKG usually shows low voltage.
Electrical alternan, if present, confirms the diagnosis (but
is often not). Also check for signs of pericarditis-diffuse
ST elevation or diffuse T wave inversions (be cautious, as
may mimic a heart attack or a juvenile pattern)
- Echocardiogram
confirms the diagnosis
- Pericardiocentesis (removal of fluid from the pericardial sac) can be used to treat the Pericardial Effusion/tamponade and the fluid can be sent to
the lab and help make the diagnosis.
- Pericardial biopsy may be necessary to determine the cause of the Pericardial Effusion
|
 |
- Treat the underlying cause (e.g.,
kidney failure is treated with dialysis, Dressler's syndrome
is often treated with nonsteroidal anti-inflammatory
medications)
- When Pericardial Tamponade occurs, urgent Pericardiocentesis is needed (removal of fluid from the pericardial sac, usually done by guiding a needle with either an EKG or an Echocardiogram)
|
 |
- Pericardial Effusions usually represent a serious medical condition, and medical treatment should be sought immediately. Cardiac Tamponade is a
life-threatening emergency, requiring immediate medical
treatment.
|
| | |
If you want your friend to read or know about this article, Click here
 |
|
|

