|
|
 |
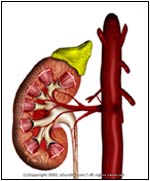
Normal |
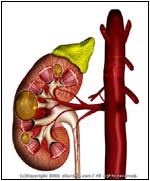
Abnormal |
| |
- PKD is a disorder characterized by the development of multiple, balloonlike sacs (cysts) in one or both kidneys. The cysts are filled mostly with fluid, but may contain semi-solid material. Over time (after many years), the cysts can replace most of the kidney and reduce its ability to remove the body's toxic wastes and reabsorb vital nutrients (i.e., renal or kidney failure).
- The accumulation of these waste materials can poison the body, and make the patient very sick (end-stage renal disease or ESRD). Over 50% of PKD sufferers develop ESRD and require dialysis (a machine that performs the filtering function of the kidneys) or kidney transplantation.
- Dialysis removes the accumulated waste by filtering the patient's blood. Transplantation is done by removing the diseased kidney and replacing it with one from a kidney donor.
|
 |
- Pain in the back or flank area (i.e., between the ribs and the lower back or hips) is seen in 60% of cases.
- Headache
- Fatigue
- Abdominal pain
- Frequent urination at nights (nocturia)
- Frequent urination all day
- Urinary Tract Infections
- Large urine volumes (polyuria)
- Children with PKD have High Blood Pressure and Blood in the Urine.
- Neonates with PKD are smaller than normal.
- Burning sensation during urination.
|
 |
- Most cases (90%) of PKD are inherited, which means PKD is passed down through genes (DNA) from parent to a child.
- The autosomal (alike in both parents) dominant pattern of inheritance -- the most common form of inheritance. One parent has the gene for PKD, creating a 50% chance that the disease will be passed on to their child. The first signs of the disease are usually seen between the ages of 30-40. The disease is also seen in childhood.
- Autosomal recessive pattern -- requires both parents to carry an abnormal variation of the PKD gene, which means that if both parents (neither actually has PKD) pass their defective gene to their child, he will have the disease. If only one parent passes his/her defective PKD gene, the child will not have PKD. The first signs of PKD appear in neonates (newborns) or even in the womb.
- Acquired cystic kidney disease (ACKD) is not inherited, and can affect individuals with long time kidney problems and those on dialysis.
|
 |
- Symptoms
- Family history
- Birth history
- Illnesses
- Surgeries
- Medications
- Allergies
- Habits
- High Blood Pressure
- Small baby
- Back pain or flank pain
- Fever if there is an
infection
- Palpable kidneys -- cystic
kidneys sometimes can be felt (palpated) by the doctor,
whereas normal kidneys cannot.
- Enlarged liver
(hepatomegaly)
- Blood samples may show evidence of kidney failure (e.g., high Creatinine, BUN, and Potassium
levels).
- Cysts may rupture or bleed -- there will be Blood in the Urine (Hematuria).
- Urine samples may show protein or
red blood cells (bleeding) in the urine.
- If there are Kidney Stones present, there may be Calcium Oxalate
crystals in the urine.
- Ultrasound (using sound waves), CAT scan (using computers), and MRI (using magnetic energy), can all show the cysts in the kidneys. These tests may also show:
- Pancreatic or Liver Cysts
- Abnormal heart valves -- mitral valve prolapse
- Kidney Stones
- Aneurysms -- blood vessels in the brain may balloon in certain areas.
- Diverticulosis --
abnormal sacs in the large intestines
- Amniocentesis -- a special technique performed while baby is in the womb to diagnose PKD
- Genetic studies and Ultrasound of close family members is recommended.
|
 |
- Family history of PKD -- genetics
- History of kidney disease
- Dialysis
|
 |
- A kidney specialist known as a nephrologist is usually consulted.
- Treat infections, blood pressure, pain, and Hematuria
- Treat ESRD with dialysis or transplantation
- Observe pregnant woman with PKD for High Blood Pressure
- Low protein diet is helpful.
- ACE inhibitors are recommended for treatment of High Blood Pressure (avoid diuretic medications).
- Genetic counseling with a specialist must be done.
- Avoid drugs that may damage kidneys.
- Drink plenty of water.
|
 |
-
Contact your physician for proper evaluation.
|
 |
- Medullary sponge kidneys
- Cysts without PKD
- Medullary cystic disease
- Renal carcinoma (cancer)
- ACKD
|
| | |
If you want your friend to read or know about this article, Click here
 |
|
|

